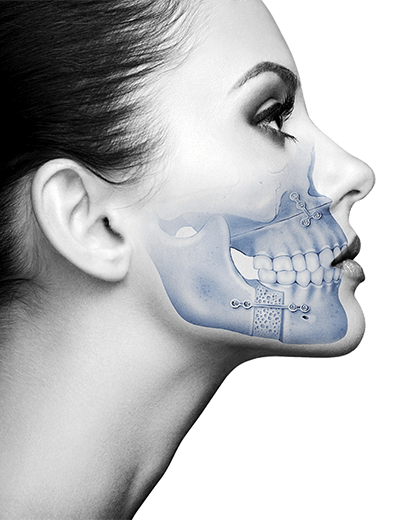
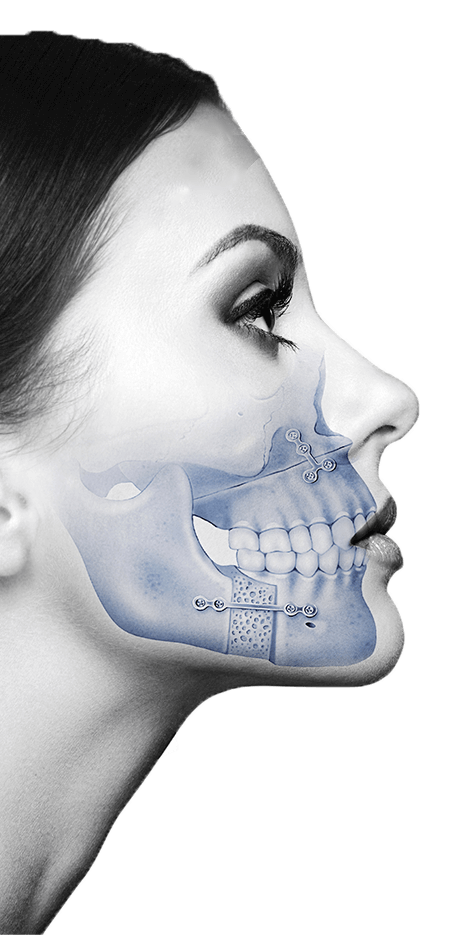
Relapse is a fear commonly expressed by patients who undergo any surgery. In the case of orthognathic surgery, there are mainly two types:
1- Dental relapse, when there is a change in the position of the teeth after surgery — this type of recurrence is the most common.
2- Skeletal relapse, when there is a change in the position of the bones- this type of recurrence is exceptional and, if it occurs, is usually too small to be considered functionally or aesthetically relevant (between 1 to 3mm)
Dental relapse is easily treatable with orthodontic treatment. Skeletal relapse occurs due to remodeling of the bones due to the muscular tensions that act on them. If this happens during the first weeks after surgery (when the bones have not yet 'welded' in their new position), revision surgery is indicated, which is done on an outpatient basis under local anesthesia and sedation.
There are also external causes for relapse, such as displacement of the plates caused by trauma, and causes inherent to the patient, such as poor healing capacity, bone weakness or TMJ disorders, which cause a greater degree of occlusal instability in the patients who suffer from them.
It is also important to bear in mind that correct planning and execution of the surgery produce more stable results over time:
- If the surgery is done in patients who are too young still in the development process, the growth will affect the final position of the bone structure. Adults also present changes in the cranial structure, but in general these changes are symmetrical, unlike changes due to growth.
- If the patient is not in a correct centric relation at the time of taking molds, the results may not be stable, so the centric bite must be taken carefully and confirmed several times to ensure that both patient's condyles are in place. settled in their respective condylar fossa.
- If there is no correct pre-surgery orthodontic preparation * or post-surgical orthodontic treatment is not followed, it is very likely that the results will be unstable. * (except in patients who are candidates for Surgery First)
Finally, it must also be considered that there are bone movements more prone to recurrence, such as orthognathic surgery for the treatment of open bite. Recurrence in these cases is mainly due to the traction exerted by the tongue, so in these cases a correct reeducation of this muscle by a speech therapist is necessary, before and after surgery.
It is important to bear in mind that beyond a year, skeletal changes are only indirectly related to surgery, since it has been shown that skeletal changes exist even in patients who did not undergo orthognathic surgery, only to a lesser degree. These changes can be the result of adaptive bone remodeling, a resumption of growth, or adaptive changes in the dentition.
In short, orthognathic surgery in general has been shown to achieve stable and clinically satisfactory long-term results in the vast majority of patients.
Related content:
Pre-surgical orthodontic decompensation: get worse to get better