Even though our patients always know in advance the procedures that will be carried out during their surgery, many of them would like to know exactly what happens once the anesthesia takes effect.
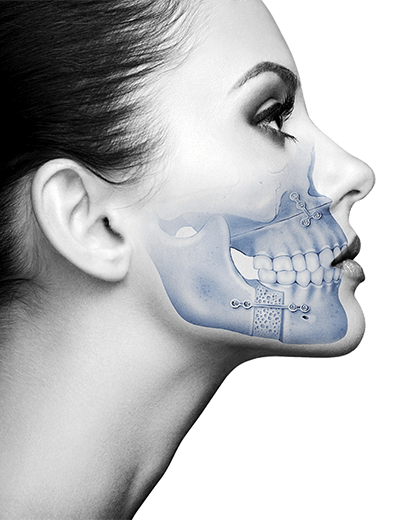
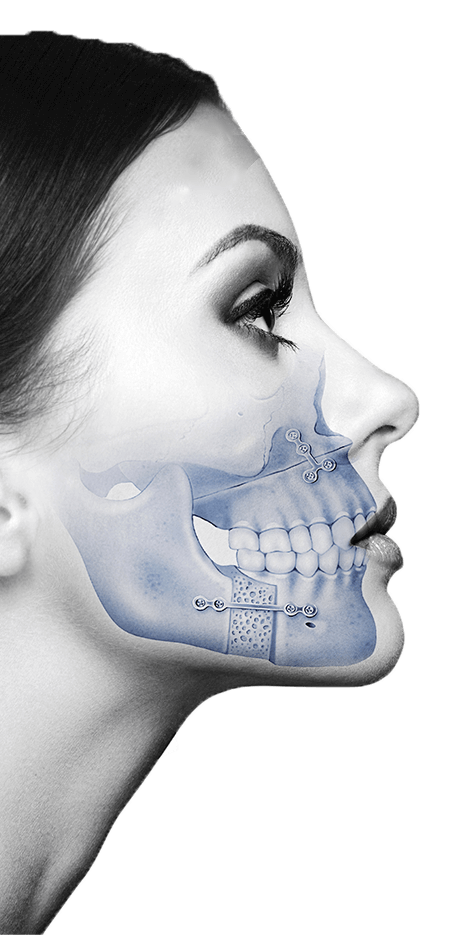
This is a step by step breakdown of a bimaxillary orthognathic surgery with general anesthesia at the Maxillofacial Institute:
After hospital admission, patients are taken to the Induction Room, where they are placed an intravenous line to administer the required drugs, as well as a soft sedative that decreases anxiety and helps the patient to relax.
Once this medication is administered, the patient enters the operating room 30 minutes before surgery. At this time, inhaled anesthetic gases are applied through a mask that plunges the patient in a pleasant state of numbness, then intubation is done.
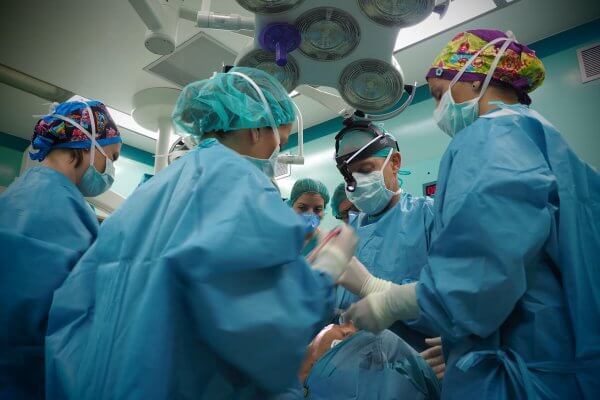
The medical team present during surgery is composed of:
- Surgeon: is the sole person in charge of performing all surgical procedures (cuts, repositioning of bones, sutures, etc.)
- First assistant: (surgeon) is in charge of the main assistantship: separation of tissues, aspiration, etc.
- Second assistant: (resident doctor) reinforcement for assistants
- Anesthesiologist : is responsible for defining the drugs (type and amount) for anesthesia, intubation and monitoring of the patient's constants throughout the surgery, as well as in the moments before and immediately after it.
- Anesthetist nurse: prepares medication, placement of intravenous line, etc.
- Instrumentalist: prepares surgical material and assists the surgeon
- Scout nurse: provides the instrumentalist material that is outside the surgical area.
- Observers: (in some surgeries) Normally medicine students, visiting doctors or in some cases the orthodontist of the patient. They are in the operating room at a safe distance from the surgical area and can not intervene for any reason.
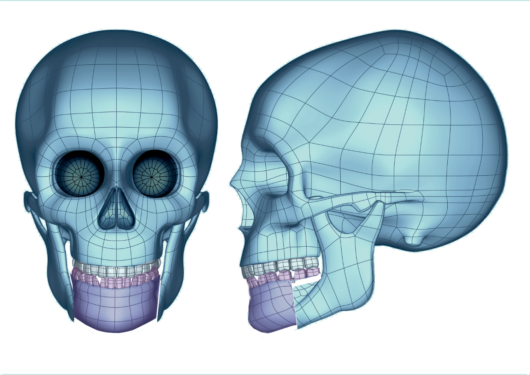
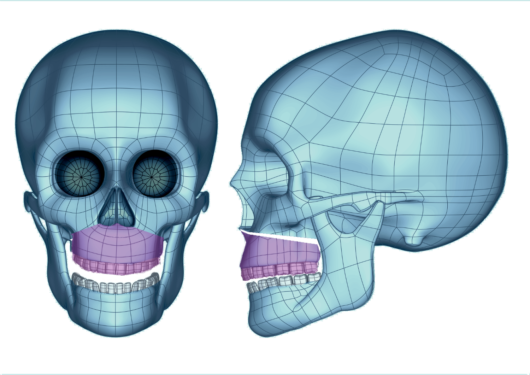
After the jaw and maxillary adjustments have been completed, if required and set beforehand, the surgeon proceeds with the ancillary aesthetic procedures required to achieve greater harmony in the face of the patient.
Related: What aesthetic procedures can one have in an orthognathic surgery?
The surgical time ends with the last suture, where previously the anesthesiologist has begun a process of decreasing anesthesia to gradually awaken the patient, a process that lasts between 10 and 15 minutes. Once patients begin to breathe on their own, the intubation tube is removed and an orderly takes the patient to the stabilization area, where they will spend approximately 2 hours under observation before going up to their hospital room to begin recovery.
It is important to emphasize that thanks to the extensive experience of our medical team, and minimally invasive techniques that we use, surgical times at Maxillofacial Institute are notably shorter than in other places, which results in a much shorter and pleasant postoperative period for the patient.
Related: Postoperative care at Maxillofacial Institute
May interest you: Everything you need to know about numbness after orthognathic surgery